Alpha-1 Antitrypsin Deficiency
Alpha-1 Antitrypsin Deficiency
Alpha-1 antitrypsin deficiency is an inherited condition occurring in approximately one in 1,200 to 2,000 live births. In this condition, the liver produces abnormal alpha-1 antitrypsin with molecules that are a different shape. This abnormal alpha-1 anti-trypsin gets “stuck” in the cells of the liver, where it accumulates, disturbs cell function and ultimately leads to liver fibrosis. Failure of alpha-1 antitrypsin to leave the liver leads to a decreased amount of the protein in blood and in other parts of the body, so its activity is low where it is needed (for example, in the lungs). A lack of alpha-1 antitrypsin in the lungs causes tissue damage, particularly in those exposed to chronic inhaled irritants, like cigarette smoke. Most people who are diagnosed with alpha-1 antitrypsin deficiency present with significant lung disease in adulthood. A small number of those diagnosed with alpha-1 antitrypsin deficiency are identified in childhood as a result of abnormalities within the liver.
What is alpha-1 antitrypsin?
Alpha-1 antitrypsin is a protein produced in the liver. One of its functions is to protect the lungs from enzymes produced by inflammatory cells, such as neutrophil-elastase. These enzymes are aimed at killing bacteria but can also cause damage to lung tissue if not properly controlled.
Causes
Alpha-1 antitrypsin deficiency is hereditary. In order to have the disease, a child must inherit two defective genes, one from each parent.
People who have only one gene for alpha-1 antitrypsin deficiency do not have the disease, but they are “carriers” of the deficiency. Their alpha-1 antitrypsin levels are lower than normal, but this does not cause any obvious health problems. In families where both parents are carriers of the gene for the disease, there is a one in four risk that a child will have alpha-1 antitrypsin deficiency.
Risk of Developing Liver Disease
For unknown reasons, only 15 per cent people with alpha-1 antitrypsin deficiency will show signs of liver disease in childhood. Of that group, about half will recover but they continue to be deficient in alpha-1 antitrypsin, putting them at risk for future complications of the disease, including lung, liver and skin disease in adulthood. The remaining 50 per cent of these children will develop worsening liver fibrosis and are at risk of liver cirrhosis and liver failure during childhood.
Adults may also develop signs of liver inflammation and liver damage later in life as the result alpha-1 antitrypsin deficiency.
Symptoms
Symptoms of alpha-1 antitrypsin deficiency most often present in one of three ways:
- As an infant who has jaundice that is caused by inflammation and obstruction of the liver cells.
- As a child or adult of any age who is found to have increased liver enzymes when blood work is drawn for an unrelated reason.
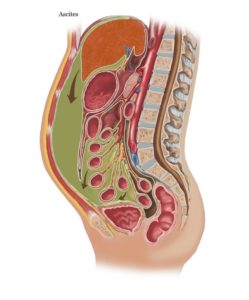
- As a child or adult of any age who has complications of liver cirrhosis including jaundice, ascites, and variceal haemorrhage.
Diagnosis
A diagnosis is established by demonstrating a very low level of alpha-1 antitrypsin in the blood and by identifying the abnormal protein in blood by specific testing. In healthy individuals the normal protein is called “M”. The abnormal protein is called “Z”.
Additional blood tests should be performed to evaluate liver function. In some cases, a liver biopsy may be needed. Breathing tests, chest x-ray and blood work may also be performed to assess lung function in those affected.
Treatment
Liver disease
Mild liver disease may need no specific treatment. As liver disease progresses, many things can help to maintain liver function and reduce complications of liver disease associated with alpha-1 antitrypsin deficiency. Examples of such therapies include good protein-energy nutrition, vitamin supplementation, management of portal hypertension and screening for varices, and the management of ascites. In rare instances where the disease progresses to liver failure, liver transplantation may be indicated as definitive treatment.
Lung disease
Over many years, injury to the lungs can result in emphysema. Typically children do not have signs of lung disease and this happens in adulthood. In some, smoking, asthma and lung infections further contribute to the development of lung disease. For this reason, it is strongly recommended that individuals with alpha-1 antitrypsin deficiency refrain from smoking and from being exposed to second-hand smoke. The symptoms of lung disease should be monitored and treated by a respirologist, a physician who specializes in lung disease.
All medical and nutritional therapies should be under the guidance of healthcare professionals.
Support
National Help Line:
This support resource gives you and your loved one somewhere to turn for answers after diagnosis, helps you understand your disease, and provides you with the resources you need. You can call 1 (800) 563-5483 Monday to Friday from 9 AM to 5 PM EST.
The Peer Support Network:
This is a national network of people living with liver disease that have offered to share their experiences with others. It was developed by the Canadian Liver Foundation as a means to link Canadians like you who have a family member who has liver disease, who care for someone who suffers from liver disease, or who have been diagnosed with a liver disease, to talk about your concerns with a peer in a similar situation.
If you would like to be connected with a Peer Supporter in your area, or would like to join the Peer Support Network, please fill out the Peer Support Network Sign-up Form.
Help us help you!
If you are not satisfied with the information you just read or any information on our website, please take a moment to send us your comments and suggestions on the type of content you would like to find on liver.ca. Please include the page you are commenting about in the subject line of your email.


